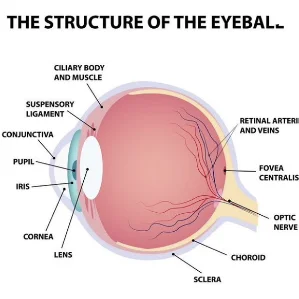
A macular pucker is a condition that occurs when the center of the retina becomes distorted or puckered, causing distortion, loss of detail, blurriness, and other issues in the patient’s vision. Whether you are dealing with macular pucker, other retinal issues such as detachment, tears, or diabetic retinopathy. Our network of doctors at Retinal Specialty Institute provides specialized care, with state-of-the-art technology and personalized treatment. Find an office near you to get started.

What Causes Macular Pucker
A macular pucker is usually caused by the formation of an epiretinal membrane (ERM), a thin film of tissue also called cellophane retinopathy, over the surface of the macula. This membrane can adhere to the macula (the part of the retina responsible for most of our color vision and fine detail) and contract, causing the macula to distort and pucker.
A macular pucker can also be caused when the posterior vitreous does not fully separate from the retina, remains or becomes adhered to the macula, and exerts varying amounts of traction or tugging on the macular tissue, resulting in puckering and distortion.
Macular Pucker Symptoms & Diagnosis
The two most common symptoms of macular pucker are distorted vision and floaters.
- The puckered or swollen macula will cause straight lines to appear curved, and if left untreated will go on to cause the central vision to fail and develop a widening spot or blurred area.
- Floaters are not directly caused by the macular pucker, but they serve as a good indicator of associated syndromes such as a retinal tear, posterior vitreous detachment, and diabetic retinopathy.
Tests that can be performed to help diagnose macular pucker include:
- A test of the macular anatomy is called Optical Coherence Tomography (OCT). OCT is the standard test to diagnose and quantify macular thickness, swelling, and distortion from the epiretinal membrane, as well as to gauge treatment effectiveness and aid in visual prognosis.
- A test of the retinal circulation called Fluorescein Angiography (FA). FA is used to complement the OCT findings and can detect subtle and specific patterns of leakage that can help to optimize treatment. To perform an FA, a fluorescent-based dye (fluorescein) is injected into your arm, and then special photos are taken of the inside of your eye. As the dye passes to your eye, more photos are taken to document blood flow and potential leakage.
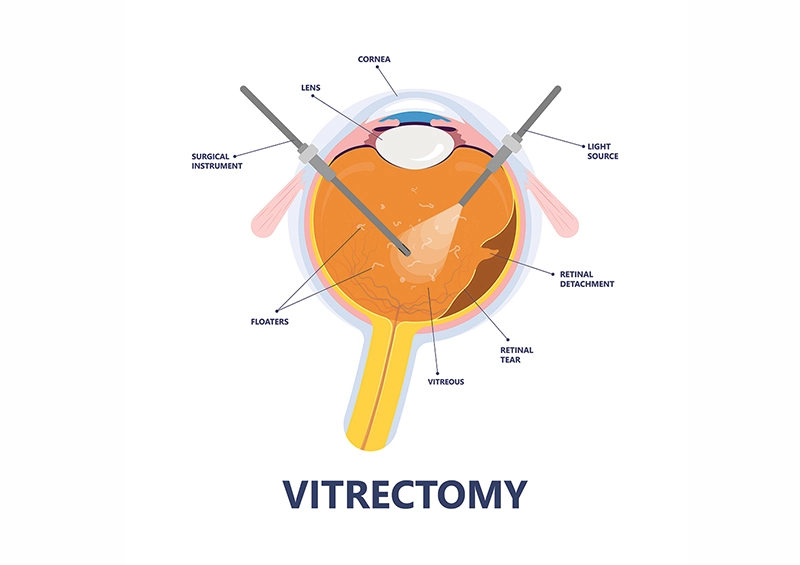
Treatment for Macular Pucker
- Vitrectomy surgery is the most direct way to address and correct a macular pucker. Although the vision does not typically return to normal, patients will see a significant improvement. This low-impact surgery removes the vitreous, thereby eliminating vitreomacular traction, and does not require stitches. Any residual retinal tissue over the macula is then removed with microscopic forceps.
- Intraocular Injections are used to treat secondary macular swelling associated with macular pucker. They can be used alone or in conjunction with vitrectomy surgery. Using injections to treat swelling alongside minimally invasive vitrectomy surgery usually accomplishes the return of vision for most patients within a few weeks of surgery.
Why Regular Medical Eye Exams Matter
Eye diseases can occur at any age, and many do not cause symptoms until the disease has done damage. Since most blindness is preventable if diagnosed and treated early, regular medical examinations by an eye doctor are very important for everyone.
Retina Specialty Institute has been involved in multiple clinical trials including studies involving vitreomacular traction. Your retinal surgeon or their staff can answer any questions you may have concerning macular pucker. Contact us to find out more.
Contact Retina Specialty Institute
Inherited retinal diseases require the treatment of a highly experienced specialist. At Retina Specialty Institute, our practice is dedicated to the treatment of all forms of retinal diseases and disorders. Our experts have deep experience in the diagnosis and management of inherited retinal diseases.
The doctors at Retina Specialty Institute have either authored or reviewed and approved this content.
Page Updated: