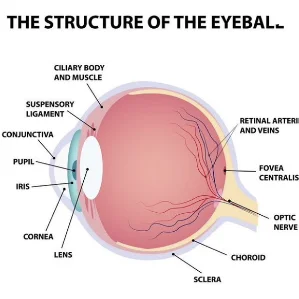
Retinal tears, holes, and detachments are serious eye conditions that can significantly impair vision or even lead to blindness. Fortunately for patients in Florida, Mississippi, Alabama, and throughout the Gulf Coast, the experts at Retina Specialty Institute are highly experienced in the diagnosis and treatment of retinal diseases and conditions.
- What is the Retina?
- What Causes Retinal Tears?
- Symptoms of a Torn Retina
- Diagnosis and Treatment of Retinal Tears
- What Causes Retinal Holes?
- Symptoms of a Retinal Hole
- Diagnosis and Treatment of Retinal Holes
- What Causes Retinal Detachment?
- Symptoms of Retinal Detachment
- Diagnosis and Treatment of Retinal Detachment
- Frequently Asked Questions About Retinal Tears, Holes & Detachment
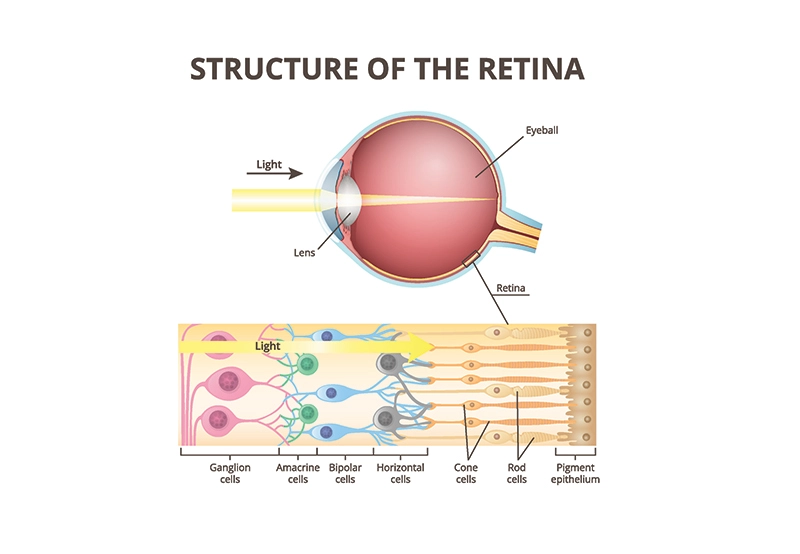
What is the Retina?
The retina is a
Trusted Source
Retina
American Academy of Ophthalmology
Go to Source
layer of light-sensitive cells
that line the back wall of the eye, separated from the lens by a jelly-like substance called the vitreous. When the lens of the eye focuses light, it is directed to the retina. The retinal cells sense the light, then send signals through the optic nerve to the brain to produce the images we see. The macula sits at the center of the retina, and is home to photoreceptor cells that help us detect color and fine details.
What Causes Retinal Tears?
A retinal tear is a
Trusted Source
What is a Torn Retina?
American Academy of Ophthalmology
Go to Source
potentially serious condition
that can cause blurry vision and may progress to retinal detachment. With the passage of time, the vitreous becomes thinner and begins to shrink. As the vitreous shrinks, it begins to pull away from the retina and may cause the retina to tear, similarly to the way cloth tears. A retinal tear may cause blood to leak into the vitreous, causing a vitreous hemorrhage. If vitreous fluid passes through a tear in the retina, it can lift the retina out of place, causing retinal detachment.
Symptoms of a Torn Retina
Patients with retinal tears may experience symptoms such as:
- Sudden flashes and/or floaters
- Blurry vision
- Shadows in the peripheral vision
- The appearance of a gray “curtain” over the field of vision
Diagnosis and Treatment of Retinal Tears
Retinal tears can be diagnosed during a dilated eye exam. It is important to treat retinal tears promptly in order to avoid retinal detachment. Treatment for a torn retina must be performed to prevent retinal detachment.
Photocoagulation
During photocoagulation, an ophthalmologist uses a laser to seal the retina against the back wall of the eye.

What Causes Retinal Holes?
A macular hole is a small hole in the macula, a small area in the center of the retina. The macula is the part of the eye that gives us much of our central vision, and it also helps us see colors and fine details.
As with retinal tears, macular holes are often a result of changes to the eye that come with age. When the vitreous thins and begins to shrink, it pulls away from the retina. Vitreous detachment is a common part of the eye’s aging process and happens to everyone. In some cases, however, the vitreous pulls on the macula when it detaches. This can cause a
Trusted Source
Macular Hole
National Eye Institute
Go to Source
macular hole
.
Symptoms of a Retinal Hole
Symptoms of a retinal hole may include:
- Blurry vision
- Visual distortion (straight lines may appear wavy)
- Dark spots or shadows in central vision
Diagnosis and Treatment of Retinal Holes
Retinal or macular holes don’t lead to retinal detachment as frequently as retinal tears do, but still require prompt treatment. Retinal holes are diagnosed through optical coherence tomography (OCT), a painless imaging technique that allows an eye doctor to see the macula in high resolution.
The most common treatment for macular holes is vitrectomy, a procedure where the vitreous is removed and a gas bubble is placed to hold the macular hole closed while it heals. If a macular hole occurs and does not significantly impact a patient’s vision,
Trusted Source
Macular Hole
American Society of Retinal Specialists
Go to Source
treatment may not be necessary
.
What Causes Retinal Detachment?
Retinal detachment is a medical emergency that may lead to total vision loss without prompt treatment.
When the retina pulls away from the back of the eye partially or fully, it has become detached. Retinal detachment is more common in people over the age of 40, though this can affect people of all ages. Retinal detachment may be caused by an eye injury or trauma, but this is not always the case and some people face a higher risk for retinal detachment.
Risk factors for retinal detachment include:
- Personal or family history of retinal detachment
- Previous eye surgery
- Diabetic retinopathy
- Myopia (nearsightedness)
-
Trusted Source Retinal Detachment National Eye Institute Go to Source Eye diseases
Symptoms of Retinal Detachment
If you have symptoms of a retinal detachment, go to the emergency room or come to our offices immediately. Retinal detachment symptoms may include:
- Sudden flashes and/or floaters
- Peripheral vision darkening
- Shadows or darkening covering part of the field of vision
Diagnosis and Treatment of Retinal Detachment
Retinal detachment can be diagnosed during a dilated eye exam. Prompt treatment is essential to preserving the patient’s vision. Surgery is necessary to treat retinal detachment and may include:
Pneumatic Retinopexy
During this procedure, the vitreous is removed and replaced with a gas bubble. The bubble is inserted to put pressure on the macula, holding the retina in place and allowing it to heal.
Vitrectomy Surgery
During vitrectomy, an ophthalmologist removes some or all of the vitreous and replaces it with a saline solution or a gas bubble to help repair a retinal detachment. As the vitreous heals, the eye naturally replaces it with a fluid called aqueous humor.
Frequently Asked Questions
About Retinal Tears, Holes & Detachment
Are there steps I can take to protect my retinas?
Technically, retinal tears, holes and detachment can’t be avoided. That said, there are steps you can take to potentially protect the health of your eyes, such as:
- Eating a healthy diet
- Not smoking
- Exercising
- Wearing goggles or protective eye gear
- Wearing sunglasses
Finally, the best way to ensure the health of your eyes is to undergo regular eye exams.
Can I prevent retinal detachment?
In many cases, retinal detachment is caused by a thinning vitreous, a natural part of the eye’s aging process. However, eye injury or trauma can also cause retinal detachment. You can decrease your risk of retinal detachment by wearing protective eyewear while playing sports or during other activities that may lead to an eye injury.

Contact Retina Specialty Institute
If you have suffered an eye injury or trauma, or if you experience symptoms of a retinal injury or detachment, seek prompt medical attention. The experts at Retina Specialty Institute maintain offices in Florida, Alabama, Mississippi, and throughout the Gulf Coast, and can quickly diagnose retinal conditions and provide potentially vision-saving treatment. Please contact us so that we can see you as soon as possible.
1 American Academy of Ophthalmology. Retina. Available: https://www.aao.org/eye-health/anatomy/retina-103. Accessed August 11, 2022.
2 American Academy of Ophthalmology. What is a Torn Retina? Available: https://www.aao.org/eye-health/diseases/what-is-torn-retina#:~:text=A%20torn%20retina%20is%20a,the%20back%20of%20the%20eye. Accessed August 11, 2022.
3 National Eye Institute. Macular Hole. Available: https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/macular-hole. Accessed August 11, 2022.
4 American Society of Retinal Specialists. Macular Hole. Available: https://www.asrs.org/patients/retinal-diseases/4/macular-hole. Accessed August 11, 2022.
5 National Eye Institute. Retinal Detachment. Available: https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/retinal-detachment. Accessed August 11, 2022.
The doctors at Retina Specialty Institute have either authored or reviewed and approved this content.
Page Updated: